Table of Contents
How we care for Severe Low Back Pain
Do it Yourself Low Back Pain Relief – Post Adjustment home protocol.
FAQ’s about Intense Low Back Pain.
Spinal Disc Conditions – What you need to know.
- Prevention and Treatment of Disc Injury – Disc Herniation, Bulging Disc, Disc Degeneration (DDD)
- What movements lead to disc injury and why, then how to avoid disc injury.
- Disc injury, Disc Age, Degenerative Disc Disease – What they mean for you and your spine.
- Disc Conditions – Centennial Chiropractor goes over each type of injury and what they mean.
Introduction
Severe spine pain and injury is possibly some of the most intense and debilitating pain you can have in your life, in our centennial chiropractic office we have even had a person crawl in on their hands and knees. Trust me it was quite a sight to see.
It goes by many names from; I’ve blown my back out, blew a disc, bent over wrong, acute disc, acute low back injury, hot low back…
Even with many names, we get a very clear mental picture of someone in intense pain, maybe even someone who is standing crooked, and/or can barely move.
Sometimes people think they are too far gone for conservative chiropractic care and jump straight to the ER or schedule an appointment with an Ortho/Neuro for injections or even surgery.
The truth is most people, even people with 10/10 pain, can start care directly with a skilled chiropractor like us. Now there are some very rare cases based on exam or history findings where we will send you straight to the ER or to an ortho/neuro spinal specialist.
A 2013 study, which looked at people with a significant spinal injury and tracked results based on the initial health care provider (chiropractor or medical doctor). A very shocking finding was people who went to the traditional medical doctor had surgery 42.7% of the time, and only 1.5% of people who started with the chiro ended up needing surgery at all.
This tells us a couple of things.
- Few people actually need surgery, often conservative chiropractic care will work great!
- If you go to a surgeon, don’t be surprised when they recommend surgery.
- There are still times when surgery is needed, but often it can be avoided.
- One route has far less risk and financial burden.
This brings up the most common question we get about serious low back cases.
“I can barely move – how are you going to work on me?”
The answer – both carefully and effectively.
When we see cases with extremely high pain levels, they can barely move, and where everything hurts our exam and care is focused solely on the problem area and is customized to that situation specifically. Our aim is to cause minimal discomfort and attain only the information needed for us to begin care that day. Only when the patient begins to improve do we do a more detailed assessment that reveals how this injury happened in the first place.
How we care for Severe Low Back Pain:

After a concise low back injury history, we start by icing the area before we even touch anything to begin numbing the pain and decreasing the sensitivity.
Then a gentle assessment of the injury, often even the assessment process can begin to be corrective and therapeutic.
Xrays are used to assess alignment, global posture, overall spine condition, disc swelling, and disc wedging.
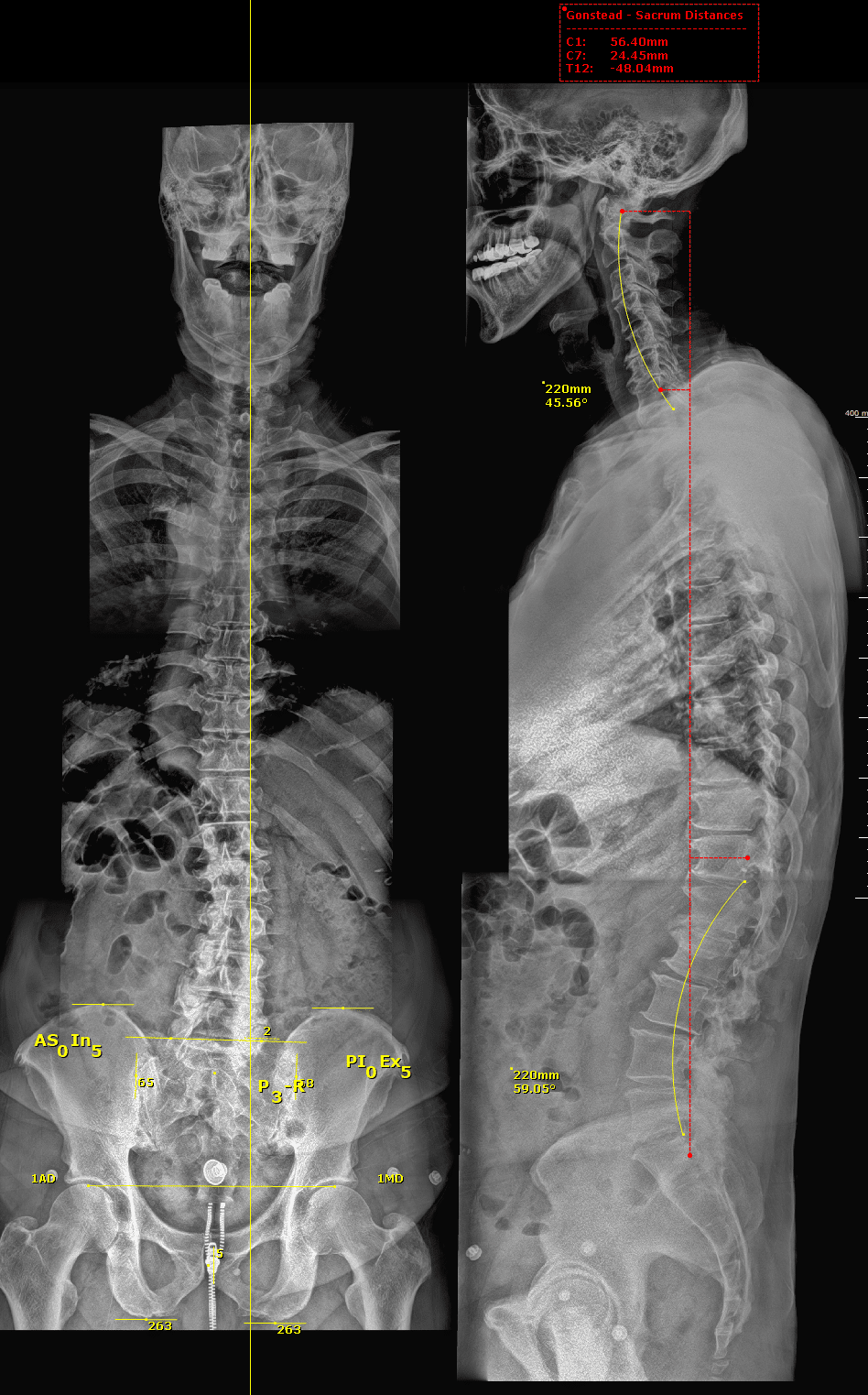
With this information, we can begin corrective chiropractic care. This process is again customized for each patient and their situation to work within their pain levels and ability to move.
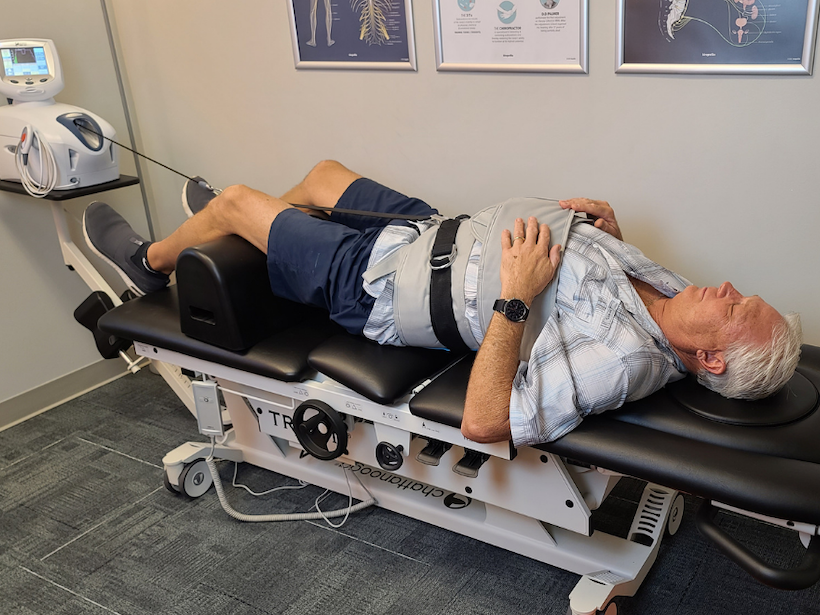
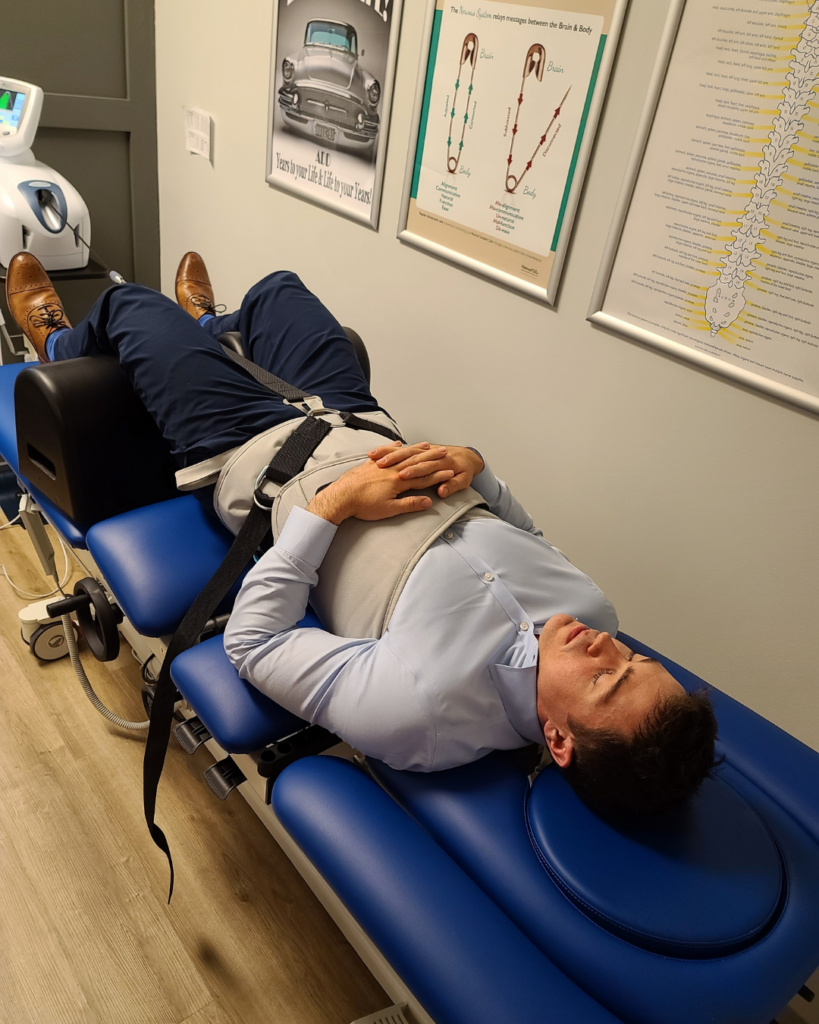
Some patients will start with gentle instrument assisted adjusting with the patient standing, sitting, or lying down. Others begin with slow and steady pressure applied by our hands to move the spine into a better position. And with some cases, we can even start with more traditional chiropractic adjustments.

Do it Yourself Low Back Pain Relief – Post Adjustment home protocol.
- Ice 20 min
- Walk 20 min
- 20min of
- Lying cobra position, pulse up and down (slowly), also add static holds in the top and bottom position.
- Lying chair position, or recovery position.
- Alternate between these positions for a 20 min period, can combine with ice as well.

Bottom of Cobra Position. With Ice Pack.


Top of Cobra Position.

Recovery Position, with an ice pack under low back.
Avoid list.
AVOID- Sitting or standing still for long periods, max sit/stand time is 50 min with 10 min of walking.
Do instead- Move for 10min every hour (frequent walks and stretching), and vary static positions ex. a lying work position.
AVOID- Spinal flexion or bending over with your back.
Do instead – use hip hinging techniques (video link)
AVOID- Compound movements – ex twisting combined with bending to the side or down to the ground
Do instead – prepare for smooth controlled movement in just one direction (just bending or just twisting), by repositioning your feet and/or pelvis.
FAQ’s about Intense Low Back Pain.
- How long till I get better?
- People typically feel better within 1-2 weeks, although some cases may be faster or slower. More serious cases can take 10-20 visits or 3-8 weeks.
- The injury itself takes about 90 days to regain stability, this number is based on muscle, tendon, ligament, bone, and nerve healing times. This number is lengthened when compounding factors are added ex. Diabetes, obesity, chronicity, older age, etc.
- How often do I need to see you?
- As often as you can – I have seen people up to 4 times in one day. The more often you can get in the faster you will get better. We begin spreading treatment frequency as soon as we can to allow greater healing time between each adjustment.
- A common example is someone who is off of work due to injury or is unable to sleep thru the night due to pain levels. For these cases, I typically see them once in the AM and once again in the PM, until they are able to return to work and sleep thru the night again.
- Why so often?
- The frequent adjustments increase blood flow thru injured areas, decreasing swelling and inflammation creating faster healing. The adjustments also stimulate the nerves, which decreases pain levels, and increases healing power.
- To avoid more serious procedures (surgery, pain pills, needle injections), to get you back to work/school/life (life doesn’t go on pause just because your hurt right?!), most importantly to get you better faster!
- What are my options
- Do nothing – the pain levels may (not always) decrease with time, but disc degeneration and spinal decay will accelerate leading to future re-injury and frequent flair-ups and exacerbations.
- Take pills (prescription or Over the counter) – may reduce temporary inflammation and numb yourself to the body’s pain signals. Both of which allow the real cause of the problem to continue to worsen. Pain medications often become addictive as well, leading to a host of other problems surrounding addiction.
- Exercise or Physical Therapy – This can be helpful with some injuries, but with spinal injuries specifically the fastest results will be obtained thru directly correcting the spinal dysfunction. It’s just like a car that is out of alignment – racing the car around the track, or “exercising” it – is not going to magically re-align the car. The only thing that is going to re-align the car is taking it to the mechanic to assess where the car is shifted out of place, then with high precision tools put it back into proper position.
- Injections – Can decrease local pain, and inflammation levels but still leaves the cause of the problem unaddressed. We must remember that the pain is not actually the problem it is a SIGN or SYMPTOM of a problem.
- Surgery – Very Expensive, and irreversible option with success rates below 50% in some cases. This should only be a last resort because anything performed is now permanent. Statistically, it is not very successful either, so much so they have a medical diagnosis code for people with a ‘failed low back surgery” (722.83 or M96.1).
- Chiropractic – Chiropractic has been proven to be the most effective means of conservative care for spine pain in countless patients and in many studies. A 2015 Systematic Review that assessed the cost-effectiveness of Chiropractic care vs Medical care (Drugs and Physical Therapy). The study reviewed over 25 separate research studies conducted over a 22-year period with 36 280 patient encounters. The review of studies found that the savings of chiropractic patients were on average $1353 or 40% less than standard medical care and had the greatest outcomes.
- How many cases like this do you see?
- In this office, we usually have 1-5 patients with very acute 8+/10 low back pain on a weekly basis. There are also many more managing chronic disc and low back conditions that were at 8+ levels and are now highly functional at work and home, with their reported pain levels varying from 0-4/10. They love that can keep feeling great and never needed surgery.
- What’s the popping noise?
- There are multiple events that can create ‘popping’ noises. The most common is if a joint hasn’t been moved in awhile it builds up pressure within the joint, when that joint is moved it can release that pressure with a sound.
- If this loss of motion is accompanied with a joint fixation or subluxation when you receive an adjustment it can also make a sound, however, this isn’t the main objective of the adjustment, merely a common side effect.
- There is one popping sound that isn’t good, see below.
- I thought popping noises were bad.
- A common story heard from people with low back pain and disc issues, is “I bent over and heard a pop, then had debilitating pain.” What happened there was a spinal bone in poor alignment, that put the disc in a compromised position (disc bulge), then the person moved in such a way that magnified the poor alignment of the spinal bone and further strained the disc to the point where the disc failed and disc fibers separated and or tore with a sound, much like a knee injury that resulted in a pop feeling and sound.
- Will adjustments hurt.
- In very acute cases, it can hurt during the process of the adjustment, but most patients begin to feel relief from their injury quickly afterward.
- What is sciatica?
- Sciatica is the name of a symptom, where there is pain that shoots from the back down the back of the leg, that can go all the way to the big toe. This is caused by compression of the sciatic nerve. The compression is created by a subluxation or joint misalignment of the lower back, a disc bulge/ herniation, a muscle spasm, or a combination of any of the previously listed.
- Do I need an MRI?
- Sometimes yes, often no. it just depends on the exam findings and your history. If they are needed we are affiliated with multiple MRI centers, so we can refer you to one that will work for you.
- How do I get in, so you can check my back out?
- Easy, click the free consultation button here. Follow the steps to get scheduled, and we will see you soon! Then you can join the ranks of the almost 2000 patients whom we have gotten well!